Work package 9
Personalized life style interventions and modulation of the metabolic milieu in the PRIL cohort
The most important mission of the health theme of the Dutch government is to decrease the disease burden of an unhealthy lifestyle and living environment with 30% in 2040. Another important mission of the Dutch government is to increase the amount of patients with a chronic disease that can participate in the society according to their wishes and ability with 25% in 2030. Whereas the previous work packages were set up to identify mechanisms of damage and repair and biomarkers for early lung damage, this work package is set up to intervene with the development diseases and extra-pulmonary manifestations at an early stage focusing on optimizing the individual’s lifestyle. This is a nested study in the PRIL-cohort. Non-invasive devices developed in WP5 might be used as part of the intervention, and life-style related risk factors suggested to correlate with respiratory disease symptoms identified in the EPIC cohort (WP1) will be considered as candidate interventions
Smoking is an important risk factor for development of lung diseases such as COPD and lung cancer, but there is increasing evidence that also other lifestyle characteristics including physical inactivity and poor dietary quality, in combination with smoking, are involved. Decreased cognitive function can diminish the susceptibility to behavioral change, aggravating disease development and affecting general health status. An optimal lifestyle is therefore necessary to decrease the development of lung diseases. Furthermore, lifestyle interventions focusing on the modulation of physical activity, diet and cognition can also deploy metabolic and endocrine actions of extra-pulmonary tissues including skeletal muscle and adipose tissue.
The aim of this work package is to test the modulating potential of lifestyle interventions to counteract or decrease the development of lung disease and associated extra-pulmonary manifestations as well as to modify overall health and well-being.
In a nested study of the PRIL-cohort, the efficacy of personalized lifestyle interventions on disease development in subjects at high risk to develop lung disease will be assessed. A personalized lifestyle intervention strategy will be based on the baseline lifestyle characteristics of individuals in the high risk group and the extra pulmonary phenotypical characteristics. Intervention will include lifestyle counseling based on preset goalsetting on smoking, physical activity level, dietary quality and cognitive performance. For development of such an intervention approach, broad experience and expertise is present within Maastricht University. The intervention will focus on long-term effects of lifestyle modification and will be assessed yearly during regular visits of the PRIL-cohort, and possibly by information passed on by wearable devices developed in WP5.
All subjects at both high and average risk to develop lung disease will be included in this nested study (Figure 8). Only half of the subjects in the high risk group (n=125) will be offered a personalized lifestyle intervention. If subjects do not want to receive a lifestyle intervention, the intervention will be offered again during the yearly follow-up visits. The other half of the subjects in the high risk group (n=125), as well as subjects in the average risk group (n=125) will be monitored yearly during the follow-up measurements of the PRIL-cohort and form the control group for this nested study. The primary outcome will be information on the development of lung disease as assessed in the PRIL cohort. Secondary outcomes will include the reversibility of biomarkers of an unfavorable metabolic milieu as defined in WP6 and overall health and wellbeing.
The deliverable of this work package is intervention strategies to counteract or decrease the development of lung disease and associated extra-pulmonary manifestations as well as to modify health and well-being.
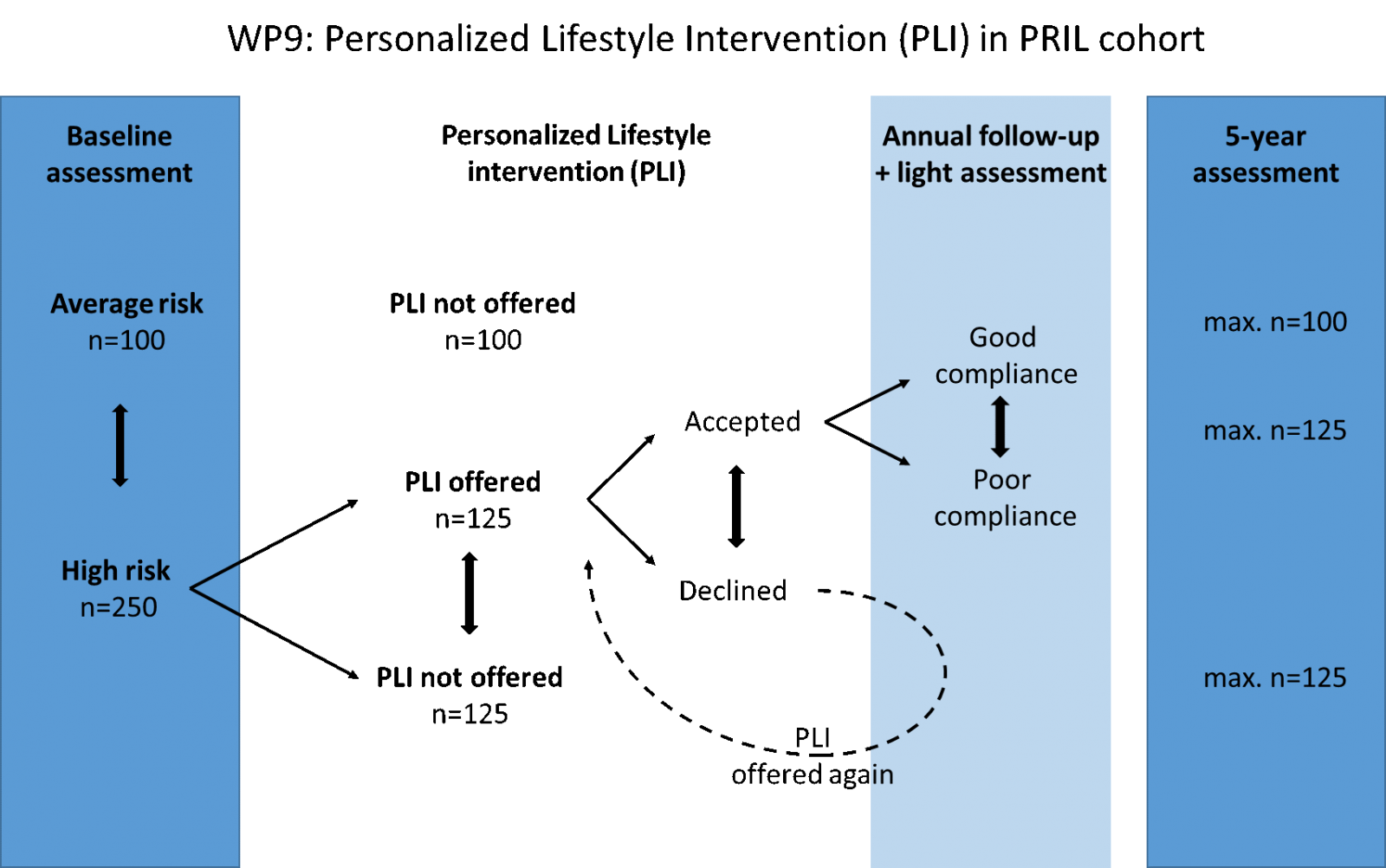
Figure 9 Set up of work package 9.
